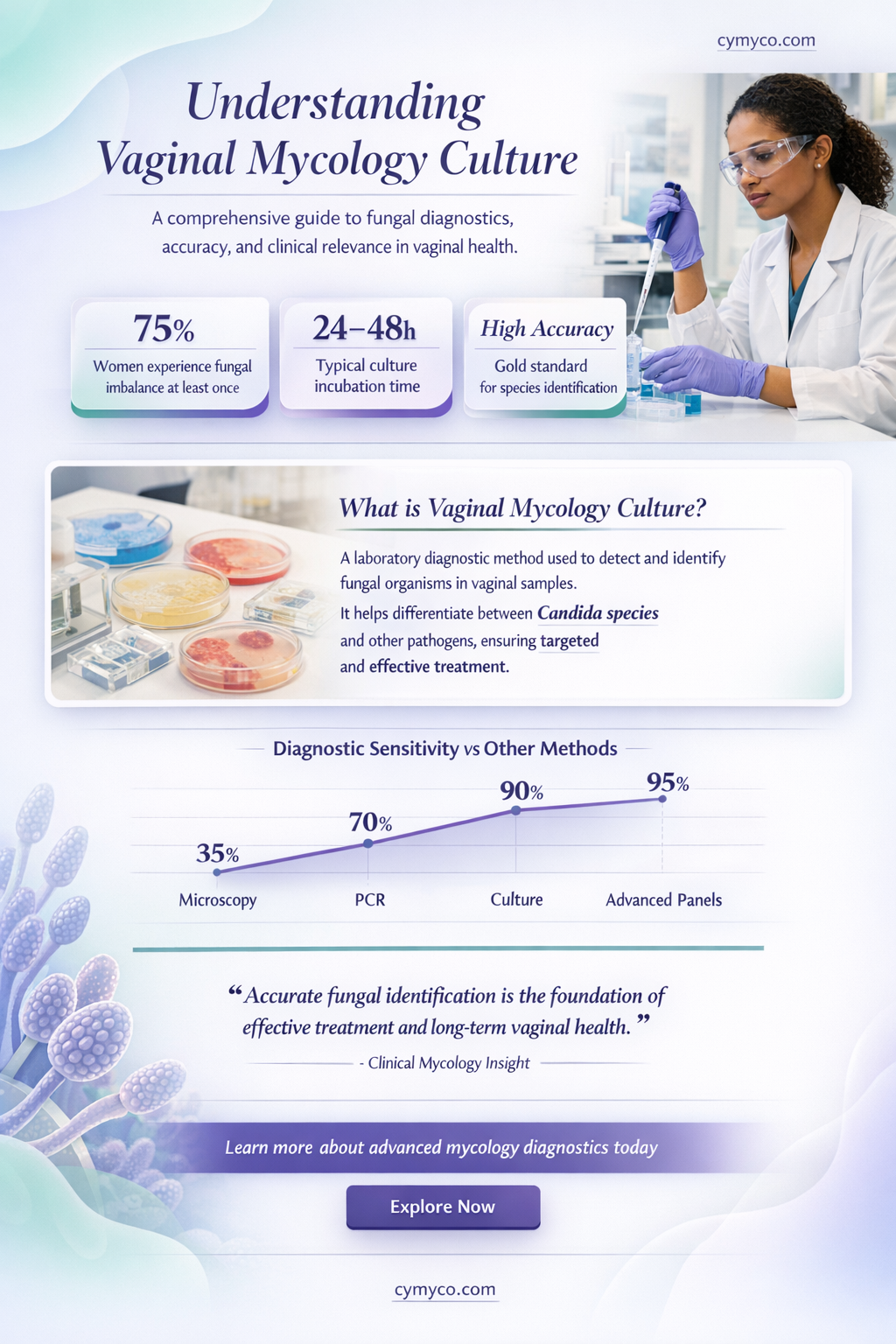
A vaginal mycology culture is a laboratory test used to identify the presence and type of fungi in the vagina. This test is typically performed when a healthcare provider suspects a fungal infection, such as candidiasis, based on symptoms like vaginal itching, discharge, or odor. The culture involves collecting a sample of vaginal discharge or tissue, which is then placed on a specialized medium in a petri dish. The sample is incubated in a controlled environment to allow any present fungi to grow. After a few days, the culture is examined to determine if fungal colonies have developed, and if so, what type of fungus is present. This information helps guide appropriate treatment, as different types of fungi may require different antifungal medications. Vaginal mycology cultures are an important diagnostic tool in women's healthcare, aiding in the accurate identification and management of fungal infections.
| Characteristics | Values |
|---|---|
| Test Type | Vaginal mycology culture |
| Purpose | To identify the presence of fungal organisms in the vagina |
| Sample Collection | Vaginal swab or scraping |
| Culture Medium | Sabouraud agar or similar selective medium |
| Incubation Period | 2-4 weeks |
| Temperature | 25-30°C (77-86°F) |
| Atmosphere | Aerobic |
| Common Pathogens Detected | Candida albicans, Candida glabrata, Candida krusei |
| Identification Methods | Macroscopic examination of colony morphology, Microscopic examination of spore structures, Biochemical tests (e.g., API Candida) |
| Reporting | Results reported as the presence or absence of fungal growth, with identification of species if present |
| Clinical Relevance | Useful in diagnosing and treating vaginal infections caused by fungi |
| Limitations | May not detect all fungal species, Culture results may take several weeks |
| Alternative Tests | PCR-based tests for fungal DNA, Immunochromatographic tests for fungal antigens |
| Preparation | No special preparation required for sample collection |
| Contraindications | None |
| Risks | Minimal risk associated with sample collection |
Explore related products
$15.99 $19.99
$18.99
What You'll Learn
- Definition: A vaginal mycology culture is a laboratory test to identify fungal infections in the vagina
- Purpose: It helps diagnose conditions like candidiasis, determining the type of fungus causing the infection
- Procedure: A healthcare provider collects a sample from the vagina, which is then cultured in a lab to grow fungi
- Results: The test results identify the type of fungus present and guide appropriate antifungal treatment
- Importance: Accurate diagnosis through culture is crucial for effective treatment and preventing recurrent infections

Definition: A vaginal mycology culture is a laboratory test to identify fungal infections in the vagina
A vaginal mycology culture is a specialized laboratory test designed to detect and identify fungal infections in the vaginal area. This diagnostic tool is crucial for healthcare providers in determining the presence of pathogenic fungi, which can cause a range of vaginal infections. The test involves collecting a sample from the vagina, which is then cultured in a controlled environment to encourage the growth of any present fungi. By examining the characteristics of the fungal colonies that develop, laboratory technicians can identify the specific type of fungus causing the infection.
The process of obtaining a sample for a vaginal mycology culture typically involves a healthcare provider using a sterile swab or brush to collect cells and secretions from the vaginal walls. This procedure is generally quick and relatively painless, although some patients may experience mild discomfort. The sample is then transported to a laboratory, where it is inoculated onto specialized growth media. These media are formulated to support the growth of a wide range of fungi, allowing for the isolation and identification of the infecting organism.
In the laboratory, the growth of fungal colonies is monitored over several days. Technicians look for specific morphological features, such as the color, shape, and texture of the colonies, to help identify the type of fungus. In some cases, additional tests may be performed to confirm the identification, such as microscopic examination or the use of biochemical assays. Once the fungus has been identified, the laboratory will report the results to the healthcare provider, who can then determine the appropriate course of treatment.
Vaginal mycology cultures are an essential tool in the diagnosis and management of vaginal fungal infections. They allow healthcare providers to accurately identify the type of fungus causing the infection, which is critical for selecting the most effective treatment. Without this diagnostic information, providers might prescribe a treatment that is not effective against the specific fungus, leading to persistent symptoms and potential complications. By using vaginal mycology cultures, healthcare providers can ensure that patients receive the most appropriate and effective care for their vaginal fungal infections.
Mold vs. Fungi: Unraveling the Differences and Similarities
You may want to see also
Explore related products

Purpose: It helps diagnose conditions like candidiasis, determining the type of fungus causing the infection
A vaginal mycology culture is a diagnostic tool used to identify fungal infections in the vagina. The primary purpose of this culture is to help diagnose conditions like candidiasis, a common yeast infection, by determining the specific type of fungus causing the infection. This information is crucial for healthcare providers to prescribe the most effective treatment.
The process of obtaining a vaginal mycology culture involves collecting a sample from the vagina using a sterile swab or brush. This sample is then placed on a culture medium, which is a substance that supports the growth of microorganisms. The culture medium is incubated in a controlled environment, allowing the fungi present in the sample to grow and multiply.
After a few days, the culture is examined for the presence of fungal colonies. These colonies can be identified based on their appearance, such as color, shape, and texture. In some cases, additional tests may be performed to confirm the identification of the fungus. Once the type of fungus is determined, healthcare providers can prescribe the appropriate antifungal medication to treat the infection.
Vaginal mycology cultures are particularly important for diagnosing recurrent or severe cases of candidiasis, as well as for identifying other types of fungal infections that may not respond to standard treatments. By determining the specific type of fungus causing the infection, healthcare providers can tailor the treatment plan to the individual patient, increasing the likelihood of a successful outcome.
In addition to diagnosing fungal infections, vaginal mycology cultures can also be used to monitor the effectiveness of treatment. By repeating the culture after a course of antifungal medication, healthcare providers can determine if the infection has been successfully treated or if further treatment is necessary. This helps to ensure that patients receive the most appropriate and effective care for their condition.
Mastering Mycology: A Comprehensive Guide to Becoming a Fungal Expert
You may want to see also
Explore related products

Procedure: A healthcare provider collects a sample from the vagina, which is then cultured in a lab to grow fungi
A healthcare provider collects a sample from the vagina using a sterile swab or brush. This procedure is typically performed during a pelvic examination. The sample is then placed on a culture medium in a laboratory, where it is incubated under specific conditions to promote the growth of fungi. The culture medium may contain nutrients and antibiotics that selectively encourage the growth of certain types of fungi while inhibiting the growth of bacteria and other microorganisms.
The incubation period for a vaginal mycology culture can vary depending on the laboratory's protocols and the type of fungi being targeted. Generally, the culture is examined daily for signs of fungal growth, such as the appearance of colonies or the production of spores. Once fungal growth is observed, the culture is further analyzed to identify the specific type of fungus present. This may involve microscopic examination of the fungal cells and the use of specialized tests to determine the fungus's susceptibility to antifungal medications.
The results of a vaginal mycology culture are typically reported to the healthcare provider within a few days to a week. If the culture reveals the presence of a fungal infection, such as candidiasis or trichomoniasis, the healthcare provider may prescribe antifungal medication or recommend other appropriate treatments. In some cases, additional testing or follow-up cultures may be necessary to confirm the diagnosis or monitor the effectiveness of treatment.
It is important to note that a vaginal mycology culture is not the same as a Pap smear or other cervical cancer screening tests. While these tests may also involve collecting a sample from the vagina, they are used to detect abnormal cells or the presence of human papillomavirus (HPV), not fungal infections. A vaginal mycology culture is specifically designed to identify and diagnose fungal infections of the vagina, which can cause symptoms such as itching, burning, and unusual discharge.
Exploring the Benefits of Distilled Water in Mycology: A Comprehensive Guide
You may want to see also
Explore related products

Results: The test results identify the type of fungus present and guide appropriate antifungal treatment
The results of a vaginal mycology culture are crucial in identifying the specific type of fungus causing an infection. This identification is key to prescribing the most effective antifungal treatment. For instance, if the culture reveals the presence of Candida albicans, a common antifungal medication like fluconazole may be recommended. However, if the fungus is identified as Candida glabrata, alternative treatments such as voriconazole or posaconazole might be necessary due to resistance to common antifungals.
Interpreting the results requires a detailed understanding of the different types of fungi and their sensitivities to various medications. Healthcare providers must also consider the patient's medical history, the severity of the infection, and any potential drug interactions when selecting a treatment plan. In some cases, additional diagnostic tests may be needed to confirm the results of the culture or to identify underlying conditions that may be contributing to the infection.
Once the appropriate antifungal treatment is determined, it is essential to follow the prescribed regimen carefully. This may involve taking oral medications, applying topical creams or ointments, or using vaginal suppositories. Patients should be advised on the importance of completing the full course of treatment, even if symptoms improve, to prevent the recurrence of the infection.
In addition to antifungal treatment, patients may be recommended to make certain lifestyle changes to help prevent future infections. This could include avoiding tight-fitting clothing, using breathable fabrics, maintaining good hygiene, and limiting the use of antibiotics unless absolutely necessary. For patients with recurrent infections, further investigation into underlying causes, such as diabetes or immune system disorders, may be warranted.
Overall, the results of a vaginal mycology culture play a critical role in guiding appropriate treatment and preventing future infections. By understanding the specific type of fungus present, healthcare providers can tailor a treatment plan that is most likely to be effective, leading to better patient outcomes and improved quality of life.
The Jar-Shaking Debate: Optimal Mycology Practices Explored
You may want to see also
Explore related products

Importance: Accurate diagnosis through culture is crucial for effective treatment and preventing recurrent infections
Accurate diagnosis through culture is crucial for effective treatment and preventing recurrent infections. This is particularly true in the case of vaginal mycology, where a precise identification of the fungal pathogen is essential for targeted therapy. A vag mycology culture involves collecting a sample from the vaginal area and culturing it in a laboratory to identify the specific type of fungus present. This process is vital because different fungal species require different treatment approaches, and misidentification can lead to ineffective therapy and potential complications.
One of the key benefits of accurate diagnosis through culture is the ability to tailor treatment to the specific pathogen. For example, Candida albicans is the most common cause of vaginal yeast infections, but other species such as Candida glabrata or Candida krusei may require different antifungal medications. By identifying the exact species, healthcare providers can prescribe the most effective treatment, reducing the risk of recurrent infections and improving patient outcomes.
In addition to guiding treatment decisions, accurate diagnosis through culture can also help prevent the spread of infections. For instance, if a patient is found to have a drug-resistant strain of fungus, this information can be used to implement infection control measures and prevent transmission to others. Furthermore, culture results can be used to monitor the effectiveness of treatment and detect any potential relapses early on, allowing for prompt intervention and management.
It is important to note that while culture is a valuable diagnostic tool, it is not without its limitations. Culture results may take several days to become available, which can delay treatment initiation. Additionally, some fungal species may be difficult to culture or may require specialized techniques for accurate identification. Despite these challenges, the benefits of accurate diagnosis through culture far outweigh the drawbacks, making it an essential component of effective vaginal mycology management.
In conclusion, accurate diagnosis through culture is crucial for effective treatment and preventing recurrent infections in vaginal mycology. By identifying the specific fungal pathogen, healthcare providers can tailor treatment to the individual patient, reducing the risk of complications and improving outcomes. Furthermore, culture results can be used to monitor treatment effectiveness and implement infection control measures, ultimately contributing to better patient care and public health.
Is Mycolog Still Available? Exploring Its Current Production Status
You may want to see also
Frequently asked questions
A vaginal mycology culture is a laboratory test used to identify the presence and type of fungi in the vagina. It involves collecting a sample of vaginal discharge and culturing it on a specialized medium to allow any fungal organisms to grow.
A vaginal mycology culture is typically performed to diagnose fungal infections of the vagina, such as candidiasis (yeast infection). It can also be used to identify other types of fungi that may be causing symptoms or to rule out fungal infections in cases where other causes of vaginal discharge are suspected.
A vaginal mycology culture is collected by inserting a sterile swab into the vagina and gently scraping the walls to obtain a sample of vaginal discharge. The swab is then placed in a specialized transport medium and sent to a laboratory for analysis.
The most common type of fungus identified through a vaginal mycology culture is Candida albicans, which causes candidiasis. Other types of fungi that can be identified include Candida glabrata, Candida krusei, and various species of Aspergillus and Fusarium.
The time it takes to get the results of a vaginal mycology culture can vary depending on the laboratory, but it typically takes 3-7 days for the culture to grow and for the results to be available. In some cases, it may take longer if additional testing is required to identify the specific type of fungus present.